Scientists warn of potential brain damage linked to COVID-19
LONDON - Scientists warned on Wednesday of potential brain damaged linked to the novel coronavirus, including severe neurological complications such as delirium, brain inflammation, stroke and nerve damage.
A study led by researchers at University College London described more than 40 patients with COVID-19 who experienced a multitude of different brain effects.
Some people in the study did not have severe respiratory symptoms, and the neurological problem was the COVID-19 patient’s first and primary symptom.
RELATED: Beyond fever and shortness of breath, experts say COVID-19 symptoms can appear in unusual ways
The study, published in the journal Brain, also identified a sometimes deadly inflammatory condition known as acute disseminated encephalomyelitis (ADEM), which appears to be increasing in prevalence due to the pandemic.
Typically seen in children, ADEM is rare and can be triggered by viral infections, experts say.
“We identified a higher than expected number of people with neurological conditions such as brain inflammation, which did not always correlate with the severity of respiratory symptoms,” said Dr Michael Zandi, a study co-author.
“We should be vigilant and look out for these complications in people who have had COVID-19. Whether we will see an epidemic on a large scale of brain damage linked to the pandemic – perhaps similar to the encephalitis lethargica outbreak in the 1920s and 1930s after the 1918 influenza pandemic – remains to be seen,” Zandi added.
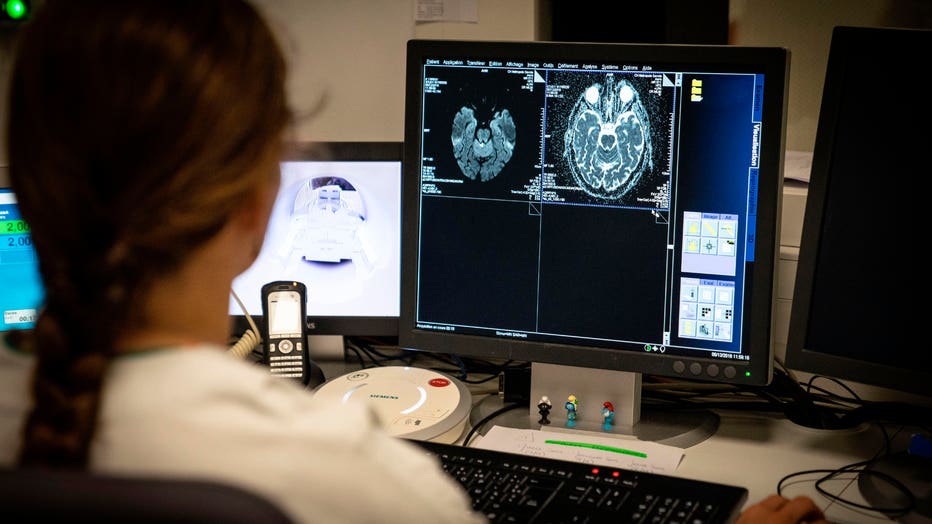
An undated file image shows a brain scan of a 77-year-old patient with signs of stroke. (Photo by: BSIP/Education Images/Universal Images Group via Getty Images)
The study described the neurological symptoms of 43 people, between the ages of 16 and 85, who were either confirmed to have or suspected of having COVID-19.
Researchers identified 10 cases of temporary brain dysfunction with delirium, 12 cases of brain inflammation, eight cases of strokes and eight others with nerve damage.
Most of those with brain inflammation conditions were diagnosed with ADEM. The team at UCL’s Institute of Neurology normally sees about one adult patient with ADEM per month, but that increased to at least one per week during the period of April and May, which the researchers said is a concerning increase.
RELATED: CoronavirusNOW.com, FOX launches national hub for COVID-19 news and updates
SARS-CoV-2, the virus that causes COVID-19, was not detected in the cerebrospinal brain fluid of any of the patients tested, the study found. This suggests that the virus did not directly attack the brain to cause the neurological illness. Further research is needed to identify why patients were developing these complications.
“Given that the disease has only been around for a matter of months, we might not yet know what long-term damage COVID-19 can cause,” said Dr Ross Paterson, a study co-author with the UCL Queen Square Institute of Neurology.
“Doctors needs to be aware of possible neurological effects, as early diagnosis can improve patient outcomes. People recovering from the virus should seek professional health advice if they experience neurological symptoms,” Paterson added.
RELATED: WHO acknowledges ’emerging evidence’ that coronavirus can spread through the air
This story was reported from Cincinnati.


